Advice from a physical therapist.
Welcome to a new series of helpful articles with valuable guidance from experts — a social-media maven, a tax guru, a costume designer and others. Check back in the months ahead for more.
In helping thousands of dancers, gymnasts and other athletes during a 22-year career, physical therapist Gregory Rakowski has used numerous methods of manual intervention. For each client, he follows up with a tailored program of exercises and neuromuscular re-education. In addition to maintaining a New York City practice, Rakowski has taught in the physical therapy program of Columbia University’s College of Physicians and Surgeons for the past 21 years.

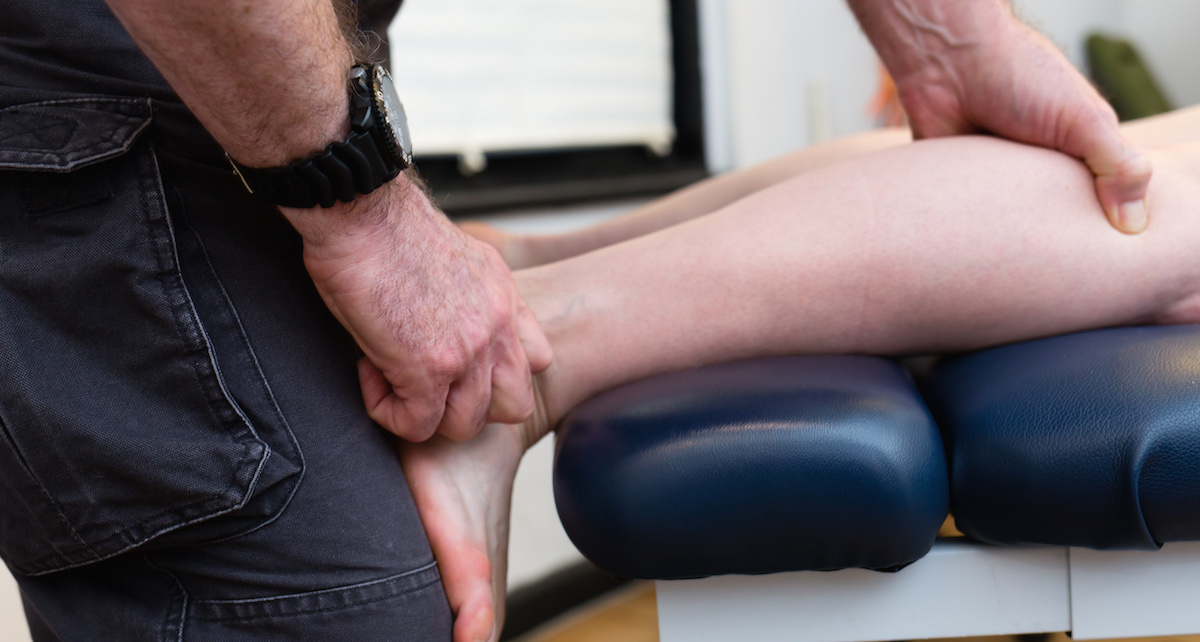
Directing the knee forward enhances this calf stretch. Photo by Joseph Zummo.
“As a dancer, you know your body well,” says Rakowski. “This means you can describe clearly what you’re feeling, and that’s great. But you dancers are also some of the most determined people around. I’ve seen you use sheer willpower to persist in doing something that’s painful and possibly damaging.”
Here are Rakowski’s top five tips for figuring out when the time has come to pause, take stock and seek help:
#1. Warning Sign
A balance problem, especially when doing something that should be easy for you, may be a tip-off that a bigger issue is brewing, Rakowski explains. The cause can vary, and your physical therapist will help you figure out what’s going on. The practitioner should begin by determining whether you have experienced physical damage that first requires medical treatment.
If the problem is not medical but is instead biomechanical or neuromuscular, the practitioner will use hands-on techniques to release the tension and rectify dysfunctions and misalignments. You’ll then get a program of exercises — and more assistance if you need it — to continue the process of releasing, realigning and stabilizing, Rakowski says.
#2. Small but Mighty
The fibula is the long, thin outer bone of the lower leg, spanning the distance from knee to ankle. It is probably not something you focus on or even know much about, because its gliding movements are so small. However, numerous ligaments and muscles of the leg attach to the fibula, making it vital for stability and range of motion, says Rakowski.
The fibula accomplishes all of this with exquisitely delicate adjustments. For example, when you flex your foot (physical therapists call this “dorsiflexion”), it glides slightly — forward at the knee and back at the ankle. When you point your foot (called “plantar flexion”), the fibula moves in contrary fashion. If the fibula isn’t gliding properly, it can sideline you.

Gregory Rakowski, or Gregory PT, as his New York City practice is known. Photo by Joseph Zummo.
How does it get stuck? Typical culprits are repeated landings from jumps and pointe work, especially with less-than-ideal body mechanics, according to Rakowski. Over time, your body builds up protective muscle tension that restricts the fibula’s minute, but critical, movements. You may feel like you have a sprained ankle. Again, you’ll need hands-on work from a physical therapist, along with an exercise program to help you correct the problem.
#3. Take Care of your Legs — Your Power Base
Additional issues of the leg will likely require assistance from a physical therapist. Rakowski sees a lot of tight calf muscles. “Most dancers live with their feet in the plantar-flexed, or pointed, position,” he explains. “Because they don’t dorsiflex enough to counter this, their calf muscles become increasingly taut.”
This exacerbates fibula problems and the movement of the talus, or ankle bone, which is the upper portion of the foot and carries the entire body weight. A practitioner can free up your calf muscles, optimizing the movement of the fibula and talus, then give you follow-up releasing work and exercises.
Another issue of the leg that Rakowski often observes is iliotibial band syndrome, or ITB syndrome. This is excessive tension in the ligament running down the outside of the thigh, as well as in an accompanying muscle called the tensor fascia latea, or TFL. The imbalance is typically painful. More importantly, he says, it inhibits the gluteus, or buttocks, muscles and can cause the kneecap to mistrack.
“ITB syndrome comes from compensation for overuse, so you can’t solve it by working harder in your familiar old pattern,” warns Rakowski. “Without effective intervention, you can end up with a downward spiral of ever-tighter iliotibial bands, non-functional glutes and possibly knee and lower back problems.”
#4. Three Strikes, and They’re Out
Speaking of practitioners, Rakowski says, “A skilled physical therapist should make a lot of headway in the problems of high-level dancers and athletes in about three sessions — or even solve them. If you don’t experience substantial improvement (and you have done your exercises), move on to another therapist.” And, he says, a physical therapist should never increase the problem or cause damage, although you might feel temporary discomfort as a result of the changes made.
The talus (ankle bone) glides to the rear as the foot flexes. Photo by Joseph Zummo.
If it turns out that you have suffered significant physical disruption, Rakowski suggests consulting an osteopath (Doctor of Osteopathic Medicine, or D.O.) or physiatrist (who may be an M.D. or a D.O.). About any surgery that’s suggested, he counsels, “Get a second, or even a third, opinion. Be certain before agreeing to this option of last resort. Once you’ve done it, you can’t go back.”
#5. Cross-Training
Both class and rehearsal can be stop and start, so you may want to add activities to build the strength and endurance you’ll need in performance. Rakowski likes fast walking, fast running, Pilates and various systems using cables or bands. “No jogging,” he warns. “It results in too much bouncing on dancers’ typically hyper-mobile joints, and that can be counter-productive or even hurtful.” He notes that stretchy vinyl rubber tubing is cheap and durable and can be easily tucked into a suitcase when you’re on the road.
“The physical therapist’s job is to get you to a place where you can improve yourself,” says Rakowski. “We show the way, and you take it from there.”
Thanks to Emily Anton, dancer with Ballets With a Twist and holistic health care professional, for modeling for us.
By Stephanie Woodard of Dance Informa.
Photo (top): The fibula spans from ankle to knee and moves in tiny, critical ways. Photo by Joseph Zummo.